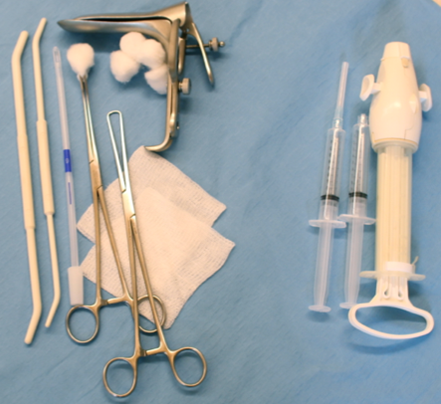
“NO-TOUCH” TECHNIQUE
Preventing infection during intrauterine procedures is an important goal. Measures to accomplish this include sterilizing instruments, administering prophylactic antibiotics, and minimizing bacterial entry into the uterine cavity by using meticulous “no-touch” technique:
- Avoid contamination by gathering needed materials before placing speculum.
- Maintain sterility of the procedure tray, separating sterile and non-sterile instruments.
- Place contaminated instruments in a separate designated “non-sterile” area of the tray.
- Do not touch any parts of sterile instruments that will be placed through the internal os. If needed, use sterile gauze to hold a dilator tip to maintain sterility.
- Attach sterile cannula to aspiration source without touching the cannula tip.
- Avoid vaginal contamination of uterine instruments.
- Change out instruments if inadvertently contaminated.
- May use non-sterile gloves, as long as “no-touch” technique is maintained.
- Even with antiseptic use, it is impossible to “sterilize” the vagina. Preoperative antiseptic vaginal cleansing has no effect on post-abortal infection rates (SFP 2025), and may decrease healthy vaginal flora without significantly decreasing endocervical bacteria.