Modern (1940’s-present)
46
Sofia Jones
Introduction
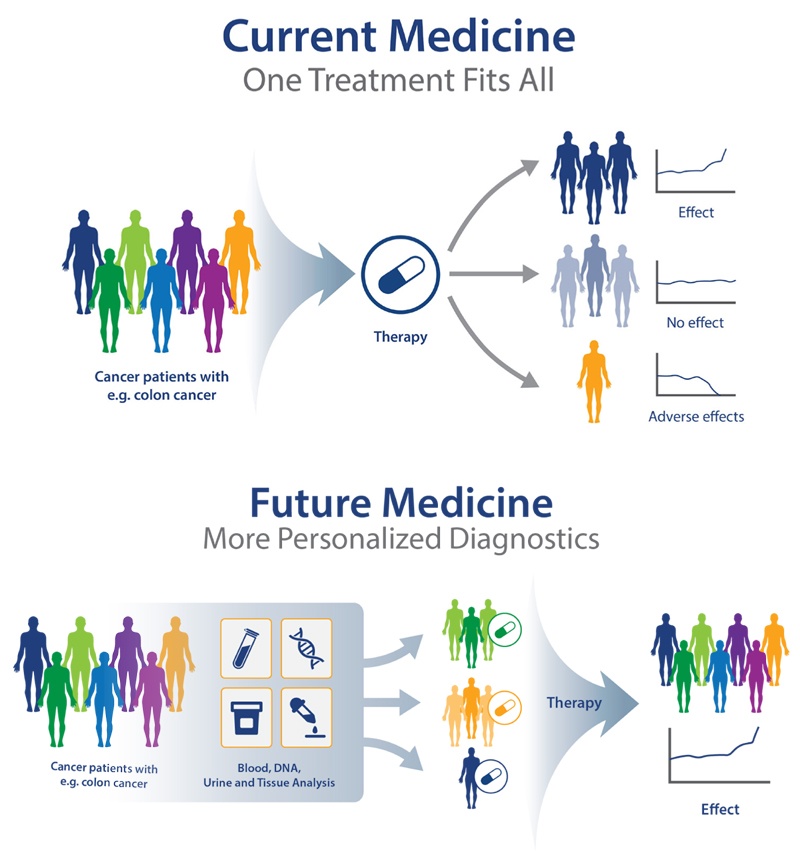 Prescription medication allows for intender patients to treat specific a specific medical diagnosis, but what if the medicine was engineered for the individual? Personalized medicine is the process of using one’s own genes to diagnose, treat, and prevent diseases which can ensuring better patient care, early treatments and diagnosis, and higher safety margins than current the prescription processes. The idea of Personalized Medicine, sometimes referred to as precision medicine, first originated in 1999 after the publishing of “New Era of Personalized Medicine: Targeting Drugs for Each Unique Genetic Profile” in The Wall Street Journal. For the first time, this article revealed the lack of efficiency in current pharmacotherapy:
Prescription medication allows for intender patients to treat specific a specific medical diagnosis, but what if the medicine was engineered for the individual? Personalized medicine is the process of using one’s own genes to diagnose, treat, and prevent diseases which can ensuring better patient care, early treatments and diagnosis, and higher safety margins than current the prescription processes. The idea of Personalized Medicine, sometimes referred to as precision medicine, first originated in 1999 after the publishing of “New Era of Personalized Medicine: Targeting Drugs for Each Unique Genetic Profile” in The Wall Street Journal. For the first time, this article revealed the lack of efficiency in current pharmacotherapy:
“Langreth and Waldholz contained several of the arguments for individualizing pharmacotherapy, as we know them, from the past 20 years of discussions. They stated that the current pharmacotherapy was a ‘one‐size‐fits‐all’ approach in which even the best drugs work in only 50%–70% of the patients” (Jørgensen, 2019).
This concept originates from the idea that diseases along with people are both heterogeneous, therefore medication would be most effective when tailored to different genes, environments, and lifestyles. Although the term wasn’t defined till 1999, the process of combining drugs and diagnosis was first done nearly 2 decades earlier when the selective estrogen receptor modulator tamoxifen was developed for treatment of breast cancer. Since then there has been an increase in the molecular understanding in the mechanism of drugs, effectively expanding the concept and practice of using personalized medicine.
Tissue Engineering
Tissue engineering, derived from the field of biomaterials engineering, consists of the artificial development of cells, skin, tissue, or even full organs typically for medical or research purposes. Although tissue engineering is still being developed and perfectioned, it has played an important role in patient treatment. One current method being used within tissue engineering is the practice of 3D-bioprinting. A research team from Tel Aviv University was able to 3D-print a functioning glioblastoma surrounded by brain tissue and functioning blood vessels. The team used biological samples from patients in order to conduct genetic sequencing of the cancer cells, which replicate the specific growth rate and behavior of each tumor. Lead researcher, professor Ronit Satchi-Fainaro, states “Cancer, like all tissues, behaves very differently in a petri dish or test tube than it does in the human body. Approximately 90% of all experimental drugs fail in clinical trials because the success achieved in the lab is not reproduced in patients” (Tel Aviv University, 2021). This achievement is a gateway for personalized medicine as different medications in multiple combinations can be tested on hundreds of bioprinted tumors to discover the optimal treatment for the specific tumor. Tissue engineering has also been involved in projects regarding ovarian cancer and even spinal cord injuries, ultimately aiming to even create functioning 3D-printed organs capable of being used for transplants.
Impact on society
Personalized medicine tackles a big discrepancy between the medical field and gender issues. While gender is a more fluid term regarding personal identity, it is important to keep in mind the biological differences between female and male sex and the impact that it can have in medication. Due to the concern that hormone variability may impact results, researchers often left women out of research studies. Until 2016 this was often also found when testing on animals as it was easier and cheaper to test on one set, typically being male. Nicole Woitoich, associate director of the Women’s Health Research Institute at Northwestern University Feinberg School of Medicine, has noted that sex influences health and treatment; however, many researchers do not look at their results by sex, making it impossible to test which drugs may impact each differently. In a recent study regarding brain tumors, Wotoich also noted how when analyzing the data by sex, it was found that they responded differently to treatments (Gordon, 2020). This is important as women are often left with undiagnosed diseases due to having different symptoms than men. With personalized medicine looking at individual’s gene structure this would completely eliminate the issue as all treatments would completely be tailored for the individual.
conclusion
Personalized medicine is a moderately new practice that holds a lot of potential for the future of medication providing access to treatments that are more effective than ever before. Personalized medicine is a gateway for rapidly functioning treatments, cutting down costs in avoidance of the “trial and error” stage of prescribed medications that will continue to develop along with technology such as tissue engineering.
Chapter Questions
- Short Answer: Where and when was the term “personalized medicine” first used?
- True or False: Prescription medication is the most effective way to treat diseases for all kinds of patients.
- Short Answer: Why might researchers need to consider sex when analyzing data?
References
Jørgensen J. T. (2019). Twenty Years with Personalized Medicine: Past, Present, and
Future of Individualized Pharmacotherapy. The oncologist, 24(7), e432–e440. Tel Aviv University. (2021, November 24). 3D printing takes on Brain Cancer. Tel Aviv
University. Retrieved December 3, 2021, from
https://english.tau.ac.il/news/3d_printing_brain_cancer. Gordon, S. (2020, June 10). Women still left out of much medical research. Medical Xpress
-medical research advances and health news. Retrieved October 23, 2021, from
https://medicalxpress.com/news/2020-06-women-left-medical.html.
Images and Media
Tel Aviv University (2021). Scientific breakthrough in the battle against cancer: First 3D printing of glioblastoma cancer tumor https://youtu.be/oUjuFyLF5nM “PDX and Personalized Medicine” by Jody Barbeau PhD is licensed under CC BY 4.0
