Chapter objectives: At the end of this chapter, the learner will:
- Identify the location of the organs contained in the abdominal cavity.
- Obtain health history relevant to the gastrointestinal or abdominal exam.
- Describe two methods (4 quadrants and 9 regions) of anatomic mapping used to describe findings related to the abdominal exam.
- Provide safety and privacy during abdominal examination.
- Perform correct techniques and order of the examination for abdominal assessment
- Document findings of the gastrointestinal system using correct medical terminology.
I. Overview of the Abdomen System
The gastrointestinal and genitourinary system is responsible for the ingestion of food, the absorption of nutrients, and the elimination of waste products. A focused gastrointestinal and genitourinary assessment includes collecting subjective data about the patient’s diet and exercise levels, collecting the patient’s and the patient’s family’s history of gastrointestinal and genitourinary disease, and asking the patient about any signs and symptoms of gastrointestinal and genitourinary disease, such as abdominal pain, nausea, vomiting, bloating, constipation, diarrhea, and characteristics of urine and feces.
II. Anatomy and Physiology
Identifying abdominal surface anatomy, 9 regions and 4 quadrants, is essential to the systematic examination of the abdomen/pelvis system. Click the link below to review anatomy and physiology of the abdominal system. You will need to apply your knowledge in the assessment process.
III. Medical Terminology
| Ascites | accumulation of fluid in the peritoneal cavity |
| Anuria | no urine; 24-hour urine output is less than 100 mL |
| Azotemia | high levels of nitrogen-containing compounds (body waste) in the blood |
| Amenorrhea | absence of menstruation |
| Blood urea nitrogen (BUN) | a blood test to check the amount of urea nitrogen |
| Creatinine | a waste generated from muscle metabolism |
| Cystocele | bulging of the anterior vaginal wall caused by protrusion of the urinary bladder through relaxed or weakened musculature |
| Diuresis | an increased excretion of urine |
| Erythropoietin | promotes the formation of red blood cells by the bone marrow; a hormone produced by the kidney |
| GERD | gastroesophageal reflux disease |
| Gravida | indicates number of pregnancies |
| Gynecomastia | abnormally large mammary glands in the man |
| Hematuria | blood in the urine |
| Hematemesis | vomiting of blood |
| Hiatal Hernia | the protrusion of the stomach through the esophageal opening in the diaphragm |
| Hypervolemia | too much fluid in the blood |
| Hypovolemia | a decreased volume of circulating blood in the body. |
| Ischemia | deficiency of blood in a particular area |
| Mastitis | inflammation of the breast |
| Melena | dark tarry sticky feces containing blood |
| Menarche | onset of menstrual cycle |
| Menopause | cessation of menses in women |
| Menorrhagia | abnormally heavy or extended menstrual periods |
| Oliguria | inadequate production or secretion of urine; 24-hour urine output less than 400 mL |
| Polyuria | excessive output of urine (diuresis) |
| Peritoneum | the serous membrane lining the cavity of the abdomen and covering the abdominal organs |
| Peristalis | the involuntary constriction and relaxation of the muscles of the intestine |
| Rebound Tenderness | pain felt when pressure as to the abdomen is suddenly removed |
| Urea | a nitrogen-containing substance normally cleared from the blood by the kidney into the urine |
| Urinary Stasis | urinary retention |
| Urinary Tract Infection (UTI) | an infection in the urinary system |
IV. Step by Step Assessment
Safety considerations:
|
|
| Steps | Additional Information |
| 1. Conduct a focused interview related to gastrointestinal and genitourinary systems. | Ask relevant questions related to the abdomen, urine output, urinary problems (hesitancy, frequency, hematuria, and dysuria), last bowel movement, flatus, any changes, diet, nausea, vomiting, and diarrhea. |
2. Inspect:
|
Abdominal distension may indicate ascites associated with conditions such as heart failure, cirrhosis, and pancreatitis.
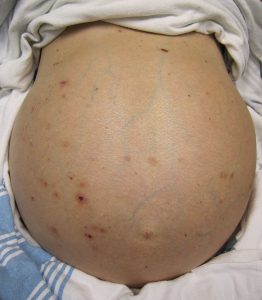 Markedly visible peristalsis with abdominal distension may indicate intestinal obstruction.
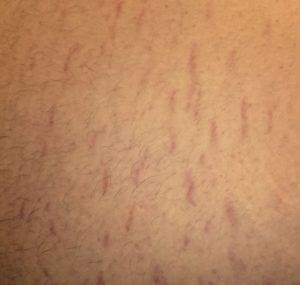
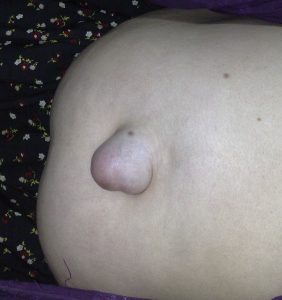 |
3. Auscultate abdomen for bowel sounds in all four quadrants before palpation. Auscultation is performed prior to palpation. It is to prevent altering the regularity of bowel sounds.
|
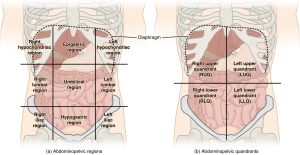
Hyperactive bowel sounds may indicate bowel obstruction, gastroenteritis, or subsiding paralytic ileus. Hypoactive or absent bowel sounds may be present after abdominal surgery, or with peritonitis or paralytic ileus. Auscultate abdomen for bowel sounds in all four quadrants |
4. Palpate:
|
Palpate to detect presence of masses and distension of bowel and bladder.
Palpate abdomen lightly in all four quadrants Pain and tenderness may indicate underlying inflammatory conditions such as peritonitis. |
| Note: If patient is wearing a brief, ensure it is clean and dry. Inspect skin underneath for signs of redness/rash/breakdown. | |
| Note: If patient has a Foley catheter, inspect bag for urine amount, color, and clarity. Inspect skin at insertion site for redness/breakdown. | |
| 5. Report and document assessment findings and related health problems according to agency policy. | Accurate and timely documentation and reporting promote patient safety. |
V. Documentation of Assessment Findings
Sample of normal findings:
Denies abdominal pain, bowel habits once a day, formed and brown; urinary patterns 4-8 times a day, denies hesitancy, dysuria, hematuria. Abdomen flat and symmetrical, midline umbilicus, no scars, skin color consistent with the rest of the body. Positive bowel sounds on 4 quadrants, soft, nontender, no distension and no guarding.
VI. Related Laboratory Values and Diagnostic Findings
Abdominal pain is the most common chief complaint related to abdominal assessment. This pain could be associated stomach/ intestine (digestion) problems, liver/gall bladder issues, pancreas problems, appendicitis (?), urinary tract problems and or problems from reproductive system. In addition to information gathered from health history and physical assessment, some laboratory tests and diagnostic exams can assist to diagnose the cause of the pain.
A complete blood count (CBC), is a blood test that can help determine if an infection is present in the body, like UTI (urinary tract infection) or peritonitis (infection of peritoneum).
Urinalysis is a urine test to determine if blood or infection is present in the urinary tract. When patients have a UTI, they may feel pain in the abdomen, or lower abdomen, and or in the back.
Liver Function Test (LFT), is a blood test to check the levels of liver enzymes. When liver enzymes are elevated, indicate a problem with the liver function.
Amylase and Lipase are blood tests to check the enzyme levels produced by the pancreas. Patient with pancreatitis will have elevated levels of these two enzymes.
Occult Stool/Hemoccult Test is a stool test. It checks the blood in stool that cannot be seen with bare eye. Positive indicates a problem (may be bleeding) in the gastrointestinal (GI) tract.
An X-ray of the abdomen (KUB) examines the kidneys, ureters, bladder, the intestines, and the bones of the pelvis and spine. Abdominal pain related to kidney stone, gas in the GI tract or constipation can be seen on the KUB x-ray.
Ultrasound uses sound waves to create images. It is often used to diagnose problems with the gallbladder or the kidneys
Computed tomography (CT) scan is used to create more detailed X-ray type images of the body.
Magnetic resonance imaging (MRI) uses magnetic fields to produce images of the body. However, it cannot be performed in patients who have metal in their body.
Esophagogastroduodenoscopy (EGD) uses an endoscope with a camera that is inserted into the mouth, esophagus, stomach and duodenum. Using this test, the GI tract (up to duodenum) can be inspected directly. This test will help to diagnose acid reflux, ulcers, or mass (cancer).
Colonoscopy, like EGD, is a test to examine the inside of the colon with an endoscope. This test will help to diagnose cancer, diverticulitis (infection of small, bulging pouches in the digestive tract), and colitis.
VII. Learning Exercises
Test your knowledge ….
- Which structure is located in the left lower quadrant of the abdomen?
A. Sigmoid colon
B. Duodenum
C. Gallbladder
D. Appendix
- The nurse is assessing a patient who may have a distended bladder. How should the nurse assess for this condition?
A. Percuss and palpate in the lumbar region
B. Inspect and palpate in the epigastric region
C. Auscultate 4 quadrants of the abdomen
D. palpate the midline area above the suprapubic bone
- A patient has experienced hematemesis. What is this? It is blood in the
A. urine
B. vomit
C. stool
D. sputum
- The nurse is performing an abdominal focused assessment on a patient who had abdominal surgery 2 days ago. How should the nurse proceed with the assessment?
A. Palpate the incision site
B. Auscultate for bowel sounds
C. Percuss for tympany
D. Inspect the abdominal area
(Correct answers are at the bottom of the chapter ….)
VIII. Attributions and References
Narayan, R. https://www.khanacademy.org/science/high-school-biology/hs-human-body-systems/hs-the-digestive-and-excretory-systems/v/meet-the-gastrointestinal-tract
Step by Step Checklist adapted from https://opentextbc.ca/clinicalskills/chapter/2-5-focussed-respiratory-assessment/ by authors Glynda Rees Doyle and Jodie Anita McCutcheon
WikiDoc editors: Gibson, C. M. & Zorkun, C. (2015). Decreased bowel sounds. Retrieved 17:36, March 25, 2021. from https://www.wikidoc.org/index.php/Decreased_bowel_sounds#cite_ref-1
Wikipedia contributors. (2019, April 8). Abdominal examination. In Wikipedia, The Free Encyclopedia. Retrieved 01:19, August 30, 2019, from https://en.wikipedia.org/w/index.php?title=Abdominal_examination&oldid=891511595
- A. Sigmoid colon
- D. palpate the midline area above the suprapubic bone
- B. Vomit
- D. inspect the abdominal area
