Chapter Objectives: At the end of this chapter, the learner will:
- Obtain the health history of the neurological system.
- Assess the neurological system of the patient including the cranial nerves, sensory function, pain, temperature, and position sense of a patient.
- Document findings of the neurological exam.
I. Overview of the Neurological System
The assessment of the neurological system include examinations of mental status, level of consciousness and examinations of the neurological function. While details of the mental status assessment will be described in the next chapter, this chapter will begin with a review of the 12 pairs of cranial nerves and their functions. It will follow by a collection of some important terminologies of this system, and then continue with key assessment components for the system.
II. Anatomy and Physiology
Click the link below to review anatomy and physiology of the neurological system. In the assessment process, you will need to apply your knowledge of the 12 pairs of cranial nerves and their functions to the neurological system.
III. Medical Terminology
The following are commonly used medical terminologies in the assessment of neurological system.
| Affect | observable behaviors that indicate a person’s feelings or emotions |
| Anxiety | a feeling of uneasiness or discomfort experienced in varying degree |
| Apathy | lack of emotional expression; indifference to stimuli or surroundings |
| Aphasia | a neurological condition in which language function is absent or impaired |
| Cognitive functioning | an intellectual process by which one becomes aware of, perceives, or comprehends ideas |
| Coherency | conversation and behavior that conveys thoughts and feelings in a logical and relevant manner |
| Cerebrovascular Accident (CVA) | a stroke; a blockage or the rupture of a blood vessel in the brain |
| Delirium | a temporary state of confusion |
| Depression | a mood disorder characterized by low mood, a feeling of sadness, and a general loss of interest in things |
| Dementia | impairment of intellectual functioning, memory, and judgment |
| Dysarthria | speech disorder involving difficulty with articulating and pronunciation of specific sounds |
| Dysphagia
Dysphasia |
difficulty in swallowing
difficulty with speech |
| Encephalitis | inflammation of the brain |
| Hyperesthesia | abnormally increased sensitivity to sensory stimuli such as touch or pain |
| Labile emotions | unpredictable, rapid shifting of expression of feelings |
| Paralysis | absence of strength secondary to nervous impairment |
| Paresis | impaired muscle strength or weakness |
| Paresthesia | numbness and tingling |
| Transient Ischemic Attack (TIA) | A neurological event with the signs and symptoms of a stroke, but which go away within a short period of time |
| Temporomandibular joint (TMJ) | the hinge joint between the temporal bone and the lower jaw |
IV. Step by Step Assessment
| Steps | Additional Information |
|
|
| 1. Obtain the health history related to mental status and the neurological system . |
Ask relevant questions related to past or recent history of head injury, neurological illness, or symptoms, confusion, headache, vertigo, seizures, recent injury or fall, weakness, numbness, tingling, difficulty swallowing (dysphagia) or speaking (dysphasia), and lack of coordination of body movements.
|
| 2. Assess mental health status, alertness and orientation, level of consciousness (LOC) general appearance, and behavior. |
|
| 3. Assess 12 cranial nerve functions.
(See chart below for more details).
|
CNI – assessing smell
CNII- assessing vision by using Snellen chart; pupillary reaction – pupils for size, equality, round, reaction to light, and accommodation (PERRLA), CNIII/IV/VI – assessing eye movement CN V – assessing jaw clench, sharp/dull sensation over three branches bilaterally CN VII – assessing raise eyebrows, smile, puff out cheeks, show teeth, squeeze eyes shut CN IX /CN X – assessing swallow CN XI – shoulder shrug CN XII – assessing tongue movement |
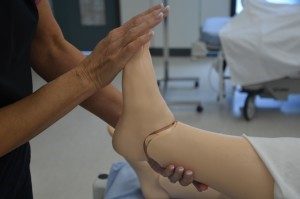
4. Assess motor strength and sensation.
|
Unequal motor strength and unusual sensation may indicate underlying neurological disease or injury, such as stroke or head injury.
Assess motor strength and sensation of extremities
|
| 5. Report and document assessment findings and related health problems according to agency policy. | Accurate and timely documentation and reporting promote patient safety. |
- Assess 12 cranial nerve functions *click all the hyper links in Assessment Column
| Mnemonic | # | Name | Function (Sensory/Motor/Both) | Assessment |
| On | I | Olfactory | Smell (S) | |
| Old | II | Optic | Vision (S) | Visual acuity Visual field Pupillary reaction |
| Olympus’ | III | Oculomotor | Eye movements (M) | Eye movements (CN III, IV, VI) |
| Towering | IV | Trochlear | Eye movements (M) | |
| Tops | V | Trigeminal | Sensory/motor – face (B) | Facial movement and sensation |
| A | VI | Abducens | Eye movements (M) | |
| Finn | VII | Facial | Motor – face, Taste (B) | Facial motor function |
| And | VIII | Auditory (Vestibulocochlear) | Hearing/balance (S) | Hearing |
| German | IX | Glossopharyngeal | Motor – throat Taste (B) | Movement of the soft palate and gag reflex (CNIX and X) |
| Viewed | X | Vagus | Motor/sensory – viscera (autonomic) (B) | |
| Some | XI | Spinal Accessory | Motor – head and neck (M) | Shrug shoulder |
| Hops | XII | Hypoglossal | Motor – lower throat (M) | Tongue |
- Glasgow Coma Scale (GCS) Assessment
Glasgow Coma Scale (GCS) Assessment is a scale to assess the level of consciousness of patients who have an acute brain injury or trauma in emergency situations. It contains assessment of three components: eye, verbal and motor responses. A fully awake person has the highest score of 15 and a person in deep coma receives the lowest score of 3.
| Response | Scale/Score | |
|
Best eye-opening response Record “C” if eyes closed due to swelling. |
Spontaneously (4)
To speech (3) To pain (2) No response (1) |
|
| Best motor response (to painful stimuli)
Press at fingernail bed and record best upper-limb response. |
Obeys verbal command (6)
Localizes pain (5) Flexion – withdrawal (4) Flexion – abnormal (3) Extension – abnormal (2) No response (1) |
|
| Best verbal response
Record “E” if endotracheal tube is in place, and “T” if tracheostomy is in place. |
Oriented x 3 (to person, time, and place) (5)
Conversation – confused (4) Speech – inappropriate (3) Sounds – incomprehensible (2) No response (1) |
V. Documentation
A sample narrative documentation:
Alert and oriented (x4) to situation, person, place, and time. Behavior appropriate to situation and developmental age. Clear speech and follow verbal commands. Cranial nerves II to XII grossly intact. Pupils Equal, Round, React to Light and Accommodation (PERRLA). Active range of motion all extremities with symmetry strength. Peripheral sensation intact.
VI. Related Laboratory Values and Diagnostic Findings
Depending on the patient’s signs and symptoms from physical examination, some diagnostic tests could be performed. For example, lumbar puncture (spinal tap) is to collect a sample of the patient’s spinal fluids to check if the patient has an infection in the brain or spinal cord or cancer in the brain. Imaging study such as magnetic resonance imaging (MRI) or computed tomography (CT) scan to diagnose a specific neurological disorder. Electroencephalogram (EEG) measures electrical activity in the brain that can be used to diagnose seizures, psychiatric disorders and other conditions of the brain.
VII. Learning Exercise
Test your knowledge …
-
- The nurse is caring for a patient who had a head injury. The patient’s respiratory and cardiac functions are affected. Which area of the brain is damaged?
A. Spinal cord
B. Brainstem
C. Cerebellum
D. Basal ganglia
-
- The nurse is documenting the physical examination findings of a patient who is unable to swallow food. The nurse will document this finding as:
A. Dysphasia
B. Dysphagia
C. Dyspnea
D. Dysarthria
(Answers and rationales to be found at the end of the chapter.)
VIII. Attributions and References
-
Courtesy of Dr. Craig Hacking and Prof. Frank Gaillard, Radiopaedia.org (https://radiopaedia.org/articles/olfactory-nerve?lang=us)
- Step by Step Checklist adapted from https://opentextbc.ca/clinicalskills/chapter/2-5-focussed-respiratory-assessment/ by authors Glynda Rees Doyle and Jodie Anita McCutcheon
- 12-Cranial Nerve function chart adapted from http://library.open.oregonstate.edu/aandp/chapter/13-3-spinal-and-cranial-nerves/#tbl-ch13_03
- Courtesy of Drs. C. Michael Gibson, Pratik Bahekar, and Sadaf Sharfaei, https://www.wikidoc.org/index.php/Glasgow_coma_scale
- National Institute of Neurological Disorders and Stroke https://www.ninds.nih.gov/Disorders/Patient-Caregiver-Education/Fact-Sheets/Neurological-Diagnostic-Tests-and-Procedures-Fact
Answers : Learning Excercises
1. Answer : B
The midbrain, pons, and medulla make up the brainstem. The medulla includes reflex centers for controlling involuntary functions such like coughing, breathing , sneezing, vomiting, and vasoconstriction.
2. Answer: B – difficulty swallowing
Dysphasia – difficulty communicating
Dyspnea – difficulty breathing
Dysarthria – difficulty in articulating and pronunciation of specific sounds