Objectives:
I. Overview: Focused Musculoskeletal System Assessment
II. Anatomy and Physiology Review:
III. Medical Terminology
Important Terms to know:
Ankylosis – fixation of a joint, usually resulting from destruction of articular cartilage
Ataxia – inability to coordinate muscular movement
Bradykinesia – abnormal slowness of movement
Crepitus – a grating, creaking, or cracking sound or sensation heard or felt when moving a join
Dyskinesia – uncontrolled, involuntary movements
Erythema – redness of the skin
Kyphosis – abnormal outward curvature of the spine
Lordosis – abnormal inward curvature of the lumbar spine
Osteoarthritis – a form of arthritis
Scoliosis – lateral curvature of the spine
Sprain – traumatic injury to the ligament
Strain – traumatic injury to the muscle or the tendon
Tendinitis – inflammation of a tendon
ROM Terms:
Abduction – movement of a limb away from the body
Adduction – movement of a limb toward the body
Circumduction – circular movement of a limb
Dorsiflexion – backward or upward motion of a body part
Extension – movement of bringing a joint into a straight position
External Rotation – or lateral rotation, turning a limb outward from the mid line of the body
Flexion – movement that brings a joint into a bent position
Hyperextension – extension of a body part beyond normal limits of extension
Internal Rotation – inward turning of a limb
Plantar Flexion – bending of the foot or toes toward the sole of the foot
IV. Step-by-step assessment of the Musculoskeletal System
A focused musculoskeletal assessment includes collecting subjective data about the patient’s mobility and exercise level, collecting the patient’s and the patient’s family’s history of musculoskeletal conditions, and asking the patient about any signs and symptoms of musculoskeletal injury or conditions. Objective data is also assessed.
The focused musculoskeletal assessment in Checklist 22 outlines the process for gathering objective data.
Focused Musculoskeletal System Assessment |
|||
Safety considerations:
|
|||
Steps |
Additional Information |
||
1. Check patient information prior to assessment:
|
Determine patient’s activity as tolerated (AAT)/bed rest requirements.
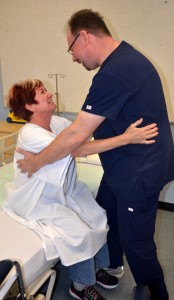 Determine if patient has non-weight-bearing, partial, or full weight-bearing status. Determine if patient ambulates independently, with one-person assist (PA), two-person assist (2PA), standby, or lift transfer. Check alertness, medications, pain. Ask if patient uses walker/cane/wheelchair/crutches. Consider non-slip socks/hip protectors/bed-chair alarm. |
||
| 2. Conduct a focused interview related to mobility and musculoskeletal system. | Ask relevant questions related to the musculoskeletal system, including pain, function, mobility, and activity level (e.g., arthritis, joint problems, medications, etc.). | ||
3. Inspect, palpate, and test muscle strength and range of motion:
Evaluate client’s ability to sit up before standing, and to stand before walking, and then assess walking ability. |
Note strength of handgrip and foot strength for equality bilaterally.
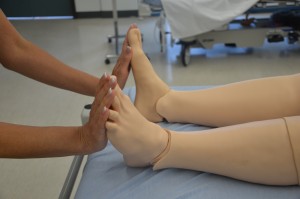 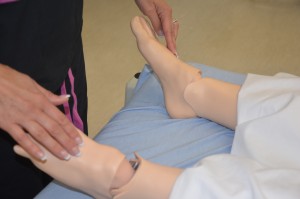 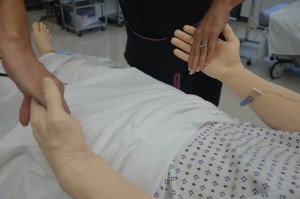 Note patient’s gait, balance, and presence of pain. |
||
| 4. Report and document assessment findings and related health problems according to agency policy. | Accurate and timely documentation and reporting promote patient safety. | ||
| Data source: Assessment Skill Checklists, 2014; Jarvis et al., 2014; Perry et al., 2014; Stephen et al., 2012; Wilson & Giddens, 2013 | |||
V. Documentation
VI. Related Laboratory and Diagnostic Tests
VII. Learning Activity
VIII. Citations and Attributions
