Caitlyn Sauls
Introduction

Living in an actual pandemic for the first time in decades is hard on anyone. No one knows exactly how to handle it. Government and public health experts in the US developed their finest protocols for containing the virus, asked society to abide by these and hoped for the best. However, it’s hard to come up with a sure-fire plan that will keep everyone completely safe and healthy. For example, no one expected that stay-at-home order, business closures and other procedures for preventing the spread of COVID-19 would decrease the state of citizens’ mental health. Governments in the US tried their best to keep the people physically healthy, but this ended up making many mentally ill. The whole pandemic situation brought about fear, stress, anxiety, and many other mental health problems. The Coronavirus and government response to it has hit those in the schooling, healthcare, and many sectors of work hard. This negatively impacted the mental health of students, healthcare workers and the working class in America.
Connection to STS Theory
This pandemic has a direct correlation with science and technology in society (STS). COVID-19 created many advances in technology, which decreased levels of physical social interaction and replaced some aspects study and work prior to the pandemic. A better definition for this is social constructivism. COVID has made it difficult to interact with people personally and easier to be in contact and do things virtually. The result of this is more advancements in science and technology which will alter society in the future. These developments makes way for a new type of adjustment society will have to take.
The Deterioration of Mental Health in Students During COVID-19
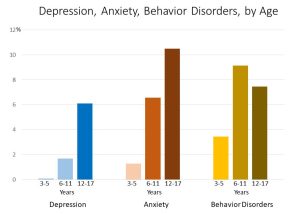
Students now have to adapt to changing circumstances in order to get their education. They’ve had to adjust to virtual at-home-learning whilst their parents are being cut from work and trying to maintain health. These conditions have led to induced stress, lack of motivation and ultimately an unstable mental health. The JAMA pediatrics network, a subgroup of the American Medical Association stated with evidence from the Centers for Disease Control and Prevention (CDC) that,
“Children and adolescents are generally healthy and do not require much health care outside of regular checkups and immunizations. However, mental health care is very important for children and adolescents. Most mental health disorders begin in childhood, making it essential that mental health needs are identified early and treated during this sensitive time in child development” (Golberstein, et al.).
The circumstances in place to keep students healthy physically is really damaging them mentally. Isolation and home-based learning often leads to children and adolescents’ social needs not being met, future behavioral or mental issues, and many technology related problems. Some students do not have the same access to secure WIFI, educated parents, or understanding concepts outside of school. College level students are having to learn real life skills from a computer, which challenges if they’re really learning or not. For example, nursing students are having to do online clinicals, simulations of work while they should be getting hands-on real-life experience. Other students struggle with learning from a computer and this has proven to be a universal problem. It also pushes stress about finances due to having to pay a full tuition for remote learning (Son). This left many college students in a sort of “slump”. Many reported no motivation, wanting to take a year off, and high levels of stress induced anxiety and depression.
Along with college level students, elementary/primary age students are also struggling with virtual learning. This is the time in their lives where they learn foundational knowledge and they cannot do it at school. Elementary school is also a vital time in their lives for developing social relationships. When the social needs of these children are not being met it can prove to be detrimental in their personalities. Younger students need that constant day-to-day social interaction in order to develop properly and older students need it as emotional relief. The lack of social interaction also plays a key part in the psyche of children and adolescents. It is easy for younger people to feel very alone during times like these, especially when they are not able to leave their homes (Terada). This has led to increased depression and feelings of being alone. It also plays a role in the connection to STS, which is the relationship between science and technology and society and how it works. Right now the average student has been advancing in use of technology but lack physical societal communication. The situation of the pandemic could potentially create new waves of technological inventions for social interaction or new social norms in the future.
Working Class at Bigger Disadvantage for Mental Health Crisis During COVID-19
The working class faced more layoffs, inability to work from home, and lack of government help, which proved to be a factor in the decline of their mental health. The working class is the majority of people, so this is a common problem for most citizens in the United States. Average working-class Americans are unable to have online versions of their jobs and often had to go back to work. Doing this posed the threat of contracting the disease and bringing it back to their families. For many working class people this was the only option unless they wanted to be fired. This financial stress was the biggest reason for the huge increase in depression among adults. There was also a constant flow of misinformation and opposing views about the pandemic. No one person in the working class genuinely knew what exactly was happening and which version of “the facts” to listen to. This caused major confusion and even more fear, which increased anxiety levels further for many working class people.
Another big thing is the fact that the stay-at-home orders had some residents feeling completely alone and isolated. Some states were more strict than others about driving or visiting family, especially in other states. Being alone and having the feeling of being isolated or abandoned can cause people detrimental harm to themselves without knowing. The fact that most of the country felt this way shows that the increased mental problems were widespread. A study by the Kaiser Family Foundation (KFF), a non-profit organization in American that researches health issues states that “Former U.S. Surgeon General Vivek Murthy has brought attention to the widespread experience of loneliness as a public health concern in itself, pointing to its association with reduced lifespan and greater risk of both mental and physical illnesses” (Nirmita et al.).
The financial stress, feelings of loneliness, and constant state of worry have deteriorated the mental health of the working class. This decline in mental health among adults in this group led to unhealthy coping mechanisms, such as aggression, substance abuse and higher rates of domestic abuse. These major stressors and increased percentage of mental health disorder was researched by KFF. They stated some of their findings that
“Many adults are also reporting specific negative impacts on their mental health and wellbeing, such as difficulty sleeping (36%) or eating (32%), increases in alcohol consumption or substance use (12%), and worsening chronic conditions (12%), due to worry and stress over the coronavirus. As the pandemic wears on, ongoing and necessary public health measures expose many people to experiencing situations linked to poor mental health outcomes, such as isolation and job loss.” (Nirmita).
However, during this time many resources were and are still available for people struggling with their mental health. These resources include healthy coping mechanisms such as exercising regularly (Mayo Clinic Staff) and reaching out to community and faith based organizations, suicide hotlines and online therapy (Centers for Disease Control and Prevention). The figure listed below shows how the percentage of adults reporting anxiety, depression, or both were constantly increasing over the months of the pandemic, specifically May through July.
Frontline Workers Face New Mental Health Challenges Due to COVID-19

Health care workers have risked not only their lives on the front lines, but also their mental health during the recent global pandemic. The increased workload, chance of catching the disease and lack of medical resources and supplies causes fear in nurses, along with anxiety and depression. The high demand for more nurses during the virus created an overwhelming workload for healthcare workers. The ratio of worker to patient is dwindling, causing difficulties for people to keep up. A study published in Journal of Clinical Nursing recently stated that “The high prevalence of COVID‐19 in the general population of many countries, its novelty and highly infectious nature, and the associated morbidity and mortality rates are placing an unprecedented demand on health and social care services worldwide” (Maben & Bridges). Many health workers stated that because of the growing patient numbers and lack of medical resources they were having to decide who gets ventilators and beds and who does not. This just adds on to their already constant responsibility of keeping people alive, which can be traumatic to some people (Maben & Bridges).
The lack of medical supplies also added to the fear of nurses and healthcare workers that they may catch the disease. The amount of personal protective equipment (PPE) was running so low at one point that nurses were using anything they could acquire. The pandemic brought on high mortality rates and more deaths at one time than most nurses have ever seen. This really took a toll on some nurses and proved to be more than they could handle. Nurses are prepared for death and illness at their job but not on such a huge scale. At one point in the pandemic there were so many patients that there weren’t enough rooms, ventilators, or even enough room in the morgue. The death rate was increasing so fast that bodies were just being collected. If they were not identified they were put in a mass grave. Many nurses saw this on a daily basis and stated that it wasn’t human. Some of them gave accounts of the mental health issues they developed as a result. One noted, “”I broke down and cried today. I cried of exhaustion, of defeat. Because after 4 years of being an ER nurse, I suddenly feel like I know nothing” (Sydni Lane, USA, Instagram and Facebook) (Maben & Bridges).
Being in an extremely demanding field that involves treating deathly ill people and with limited resources is taking a toll on healthcare workers. In addition to their extreme work environment, they often could not go home to be with their families for fear that they’d spread the virus to family members. Many nurses became extremely overworked, over stressed, and mentally fragile. Some even committed suicide. The most popular account of this was the case of Dr. Lorna Breen, an emergency doctor in New York. She contracted COVID-19 while treating large number of patients, and committed suicide when she felt that she could not keep up with her environment any further (Watkins, Ali et al.) Dr. Breen did what numerous other healthcare workers have done when they could not cope with their mental health problems. Sadly, this is the reality for healthcare workers right now. The job is getting strenuous, with no endpoint in sight and it is scary for these brave men and women.
Conclusion
COVID-19 has had a direct impact on the mental health of everyone around the globe. However, America had it particularly hard considering it had higher death rates than any other nation. Though everyone was impacted, students, health care workers, and the working class were hit the hardest, particularly in their mental health. Students struggled to grasp online learning and a lack of social interaction, which led to induced stress, anxiety, and lack of motivation. The working class dealt with financial struggles, isolation, and contradicting news on the virus, which led to increased state of fear, confusion, anger, and depression. Healthcare workers had an extreme workload, lack of resources, and risked their own health for the sake of the people. This led to burnout, depression, and in some cases an increase in suicide rates.
These are the people who, aside from COVID-19 patients, were most affected the most by the pandemic. In order for them to go on living their lives they have risked their mental health. These groups have undergone more anxiety, depression, and psychotic disorders than any other group in America. Mental health issues have a direct relation to science, technology and society because the pandemic has altered people’s lifestyles and made them more dependent on technology. People’s lives are also being restricted by scientific measures aimed at preventing the spread of COVID-19. Science and technology designed to deal with the pandemic are impacting the mental health of many people. They, along with the pandemic itself will have effects on society for years to come.
References
Centers for Disease Control and Prevention. “Mental Health and Coping During COVID-19.” Centers for Disease Control and Prevention, 1 July 2020, www.cdc.gov/coronavirus/2019-ncov/daily-life-coping/managing-stress-anxiety.html.
Mayo Clinic Staff. “COVID-19: How to Manage Your Mental Health during the Crisis.” Mayo Clinic, 2 Apr. 2020, www.mayoclinic.org/diseases-conditions/coronavirus/in-depth/mental-health-covid-19/art-20482731.
Golberstein, Ezra, et al. “Coronavirus Disease 2019 (COVID-19) and Mental Health for Children and Adolescents.” JAMA Pediatrics, vol. 174, no. 9, 2020, pp. 819-820. jamanetwork-com.libproxy.clemson.edu/journals/jamapediatrics/fullarticle/2764730.
Maben, Jill, and Jackie Bridges. “Covid‐19: Supporting Nurses’ Psychological and Mental Health.” Journal of Clinical Nursing, vol. 29, no. 15-16, 2020, pp. 2742-2750. https://onlinelibrary.wiley.com/doi/full/10.1111/jocn.15307.
Nirmita Panchal, et al. “The Implications of COVID-19 for Mental Health and Substance Use.” Kaiser Family Foundation, 21 Aug. 2020, www.kff.org/coronavirus-covid-19/issue-brief/the-implications-of-covid-19-for-mental-health-and-substance-use/.
Son, Changwon, et al. “Effects of COVID-19 on College Students’ Mental Health in the United States: Interview Survey Study.” Journal of Medical Internet Research, vol. 22, no. 9, 2020, pp. 1-4. https://www.jmir.org/2020/9/e21279/.
Watkins, Ali et al. “Top Doctor Who Treated Virus Patients Dies by Suicide”, New York Times, 27 April 2020, https://www.nytimes.com/2020/04/27/nyregion/new-york-city-doctor-suicide-coronavirus.html
Terada, Youki. “Covid-19’s Impact on Students’ Academic and Mental Well-Being.” Edutopia, 24 Jun. 2020, www.edutopia.org/article/covid-19s-impact-students-academic-and-mental-well-being.
Images
“Experiencing COVID-19: We Discuss Testing, Symptoms, Treatment, Recovery & Immunity” by Cindy Han is in the Public Domain, CC0
“Data and Statistics on Children’s Mental Health” by Centers for Disease Control and Prevention is in the Public Domain, CC0
“Screenshot of Dr. Lorna Breen Taken from her Twitter account” by Yang Wu is in the Public Domain, CC0
