Staples for Wound Closure
Step 1: Health history and physical assessment
Assess mechanism of injury and environment in which injury occurred, time of injury, site and type of wound, and medical history. Never close a wound that is more than 24 hours old.
Assess for risk factors for poor wound healing:
• impaired nutritional status
• advanced age
• medications
• diabetes
• peripheral vascular disease
• autoimmune disease
• immunosuppression
• COPD
• CHF
• anemia
• smoking
• substance use
Physical assessment:
• circulation, sensation and movement distal and proximal to the wound
• 2-point discrimination
• sharp/soft discrimination
• pulses
• capillary refill
• range of motion and strength against resistance of all body parts surrounding the wound site
• pain
Step 2: Set up equipment, wash hands, don gloves
Step 3: Cleanse wound or skin of the operative site with normal saline
Wound irrigation and debridement can be painful for the patient and may be better tolerated after the wound is anesthetized. Wound cleansing reduces the risk of sepsis to the wound site. Cleanse a wide area around the wound to prevent contamination of suture material and surgical instruments during the procedure.
Note that some antiseptics (i.e., chlorhexidine, iodine) are cytotoxic and damage fibroblasts essential to wound healing. Do not introduce antiseptic solution directly into the wound. The wound itself should be cleansed or debrided with sterile normal saline only. Alternative methods for wound debridement are below.
(a) Irrigation: Use an 18-gauge catheter attached to a 30 mL syringe. 10 PSI of irrigating pressure is needed to dislodge contaminants and bacteria, yet not damage tissue.
(b) Scrubbing: Use a sponge or a brush to remove embedded debris. Avoid soaps or detergents.
(c) Debridement: Remove retained debris and devitalized tissue by surgical excision to improve wound healing time and prevent disfigurement.
Step 4: Clip hair on surrounding skin surface
Hair surrounding the wound should be clipped rather than shaved to prevent further trauma to the skin.
Step 5: Drape the wound
Step 6: Anesthetize the wound
Step 7: Approximate and evert wound edges
Have an assistant evert and reapproximate skin edges. The stapler has a tendency to invert the wound edges impacting cosmetic appearance of the scar.
Step 8: Begin at one end of the laceration
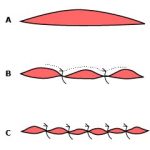
Step 9: Place staples into skin
Place stapler perpendicular to the wound. Gently hold stapler against the skin surface. Take care not to indent the skin.
Press down the handle to place the staple into the skin. Release the handle to disengage the staple. When properly placed, the crossbar of the staple is elevated a few millimeters above the skin surface to allow for swelling of the tissue.
Space staples approximately 0.5 to 1 cm apart.
Step 10: Assess tetanus status
A tetanus booster dose is required if the patient has not had a tetanus booster in the last 10 years. The combined preparation of tetanus and diphtheria toxoid formulated for adults (Td) is preferred.
If the patient has not received pertussis since childhood, then tetanus, diphtheria, pertussis (TdP) should be given. If the wound is excessively dirty, tetanus immune globulin should also be given. See Tetanus immune globulin in the Canadian immunization guide (recent edition) for further information.
Step 11: Consider prophylactic antibiotics
• more than six hours old
• the result of human or cat bites
• a crushing wound
• grossly contaminated
• bone/joint involvement
• patient is immunocompromised