CLINIC PREPARATION
Staff Communications and Training
Prior to expanding services, training and communicating with staff is vital for success. (See Ch 10: Training Staff for New Services) Important groundwork includes training staff in these areas:
- Values exploration to demystify fears and discuss concerns (see Ch 1 Exercise 3.1 – 3.3, and Ch 12 Exercise 1).
- Logistic preparations, such as changes in appointment screening and scheduling needs
- Counseling training to include navigating delays, prolonged travel, financial stressors, additional cervical preparation, and potentially difficult fetal diagnoses
- Intraoperative ultrasound skills, as evidence supports routine US for procedural abortion >14 w EGA (NAF CPG 2022, WHO 2012)
- IV starts and sedation-related administration and monitoring
- Procedure room setup
- Additional preparation staff examining fetal tissue
- Recovery processes and times
- Emergency drills with advancing gestational ages (See TEACH Simulations)
Building Skills to Incrementally Expand Abortion Care
While guided in-person training with an experienced provider is the gold standard for expanding a skill set to include instrumentation and evacuation of the uterus (NASEM 2018), non-traditional training methods may be helpful in the evolving landscape with more limited training opportunities and increased demand for abortions later in pregnancy. Simulation models for D&E (Baldwin 2013) and complications (Goodman 2015) may improve patient safety, enhance stress readiness, and reduce case numbers needed to achieve competency. Independent and stepwise increases in gestational age offerings may also allow clinicians to gradually expand provision while incrementally broadening their procedural skill set, even when opportunities to train under a more seasoned provider are limited or absent.
To establish confidence and skill with abortions ≥ 14 weeks with limited or absent training supervision by an experienced provider, it can help to establish a timeline for gradually increasing gestational age offerings with your clinic, generally by 3 or 4 day gestational increments over time. For example, increasing from ≥ 14 weeks to 14w3d will not require vast changes to procedural technique. After adequate patient volume to ensure clinician proficiency and clinic flow, the provider and clinic could increase to 15w, then to 15w3d, then to 16w, etc.. Incremental increases can allow providers to become comfortable with cervical preparation, greater dilation, and gradual introduction of forceps. Competency is best evaluated with competency-based criteria rather than number of procedures performed (See Ch 13 Observed Performance Assessment and Core Competencies), and decisions of when to increase in a stepwise fashion can be assessed by clinician comfort, case reviews with a remote mentor or supervisor, and the clinic. Alternatively, a clinic may opt to increase by larger increments (eg: 1-2 gestational weeks at a time) to allow adequate volume for clinicians to achieve and maintain procedural experience.
Instruments and Supplies
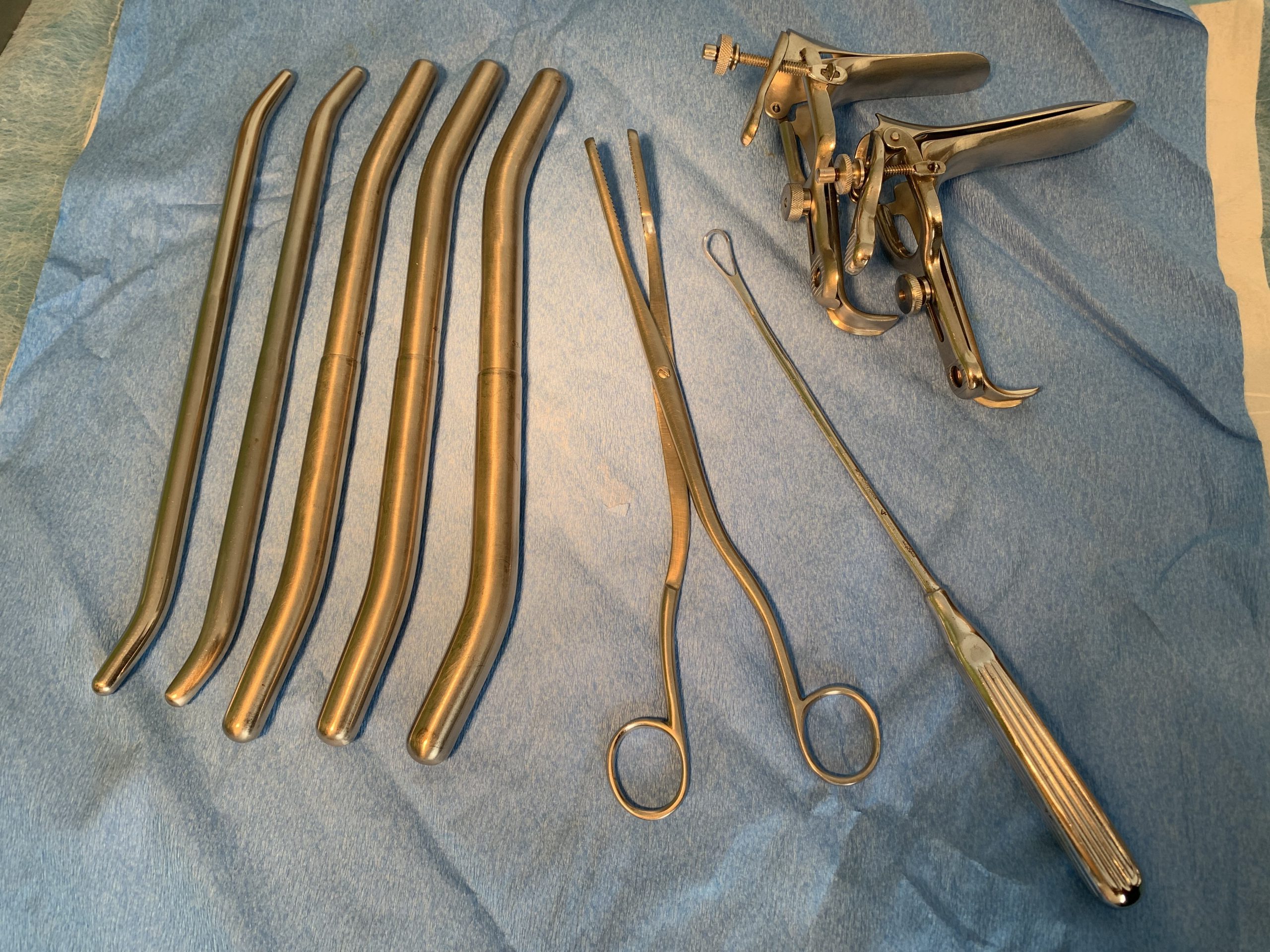
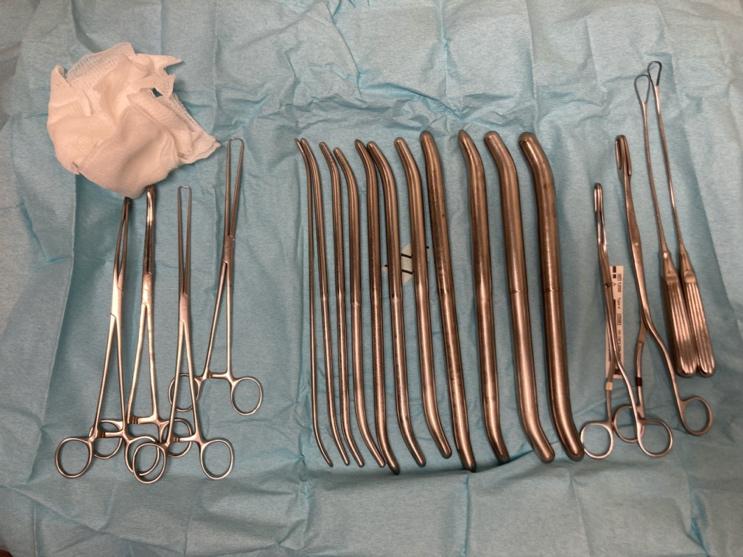
Beyond standard equipment for aspiration abortion < 14 weeks, the instruments and supplies shown below, and listed in Appendix A are suggested for abortion between 14 – 18 weeks.
Scheduling Considerations
- Telephone Screening: To minimize fragmented patient care, it is important to identify conditions influencing a patient’s eligibility for care in your facility, or indicate need for a higher level of care (e.g. history of bleeding disorders or multiple cesarean sections).
- Scheduling: Appointments for abortions starting at ≥ 14 weeks EGA will likely require more time and may be accommodated by scheduling patients earlier in the day. Generally, to allow for ultrasounds, IV starts, and cervical preparation, patients presenting for same-day D&E procedures should be scheduled from 7-10 am start time to complete their procedure by end of the clinic day. Consider the needs of patients traveling for abortion care, although some smaller volume clinics choose to “group” patients at a higher gestational age when a more experienced provider is available, to ensure that the clinician maintains skills with an adequate caseload.
- Patient flow: Consider rooms to accommodate patients undergoing cervical preparation, monitoring and abortion recovery. Ideally, patients will have space with a recliner, heating pad, and staff support away from the general waiting area for pre- and post-procedure care. (See Abortion Aftercare)