PREGNANCY OF UNKNOWN LOCATION (PUL) EVALUATION
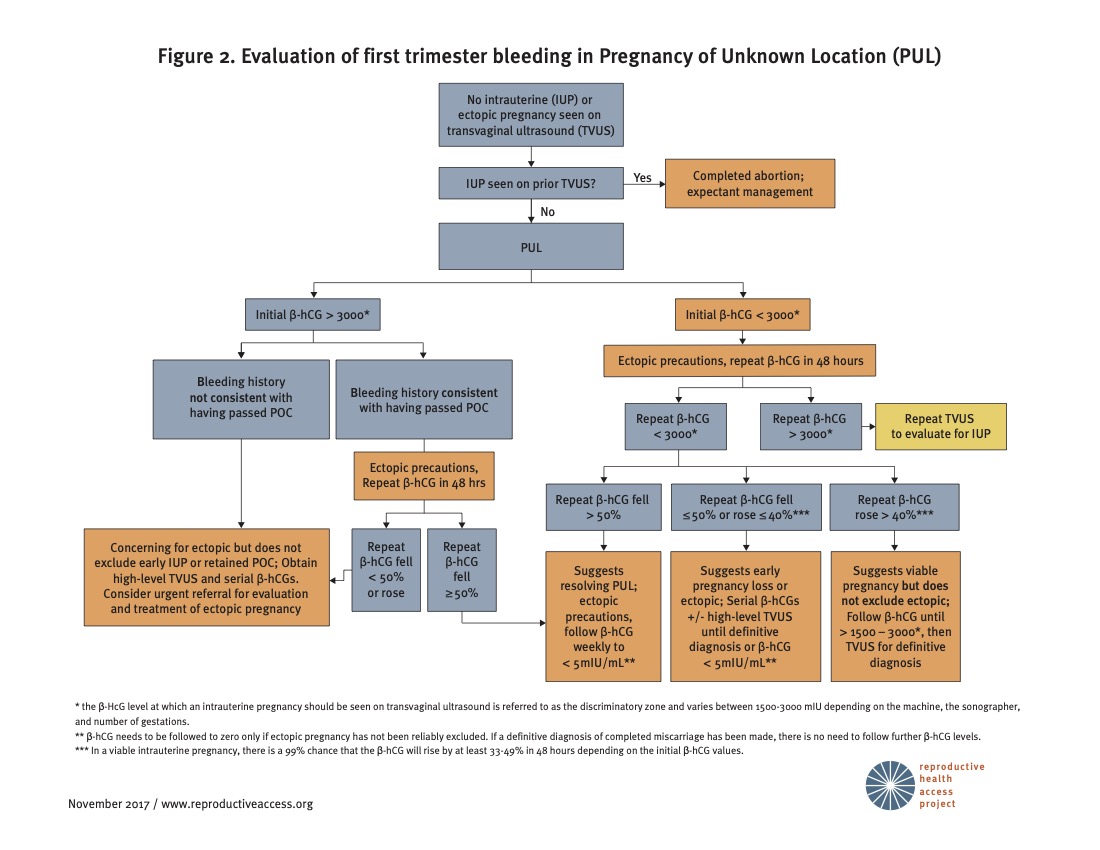
A patient with a positive pregnancy test and no visible pregnancy on US is said to have a pregnancy of unknown location (PUL). The differential diagnosis for PUL includes early viable intrauterine pregnancy, EPL, or ectopic pregnancy. Patients with PUL should be followed until a diagnosis is made. Patients may present in early pregnancy with symptoms of bleeding and / or pain and require evaluation for ectopic pregnancy according to local protocol—for example with US, serial hCGs, exam and / or diagnostic aspiration. Referral for formal diagnostic US and / or emergency attention may be indicated.
PUL DIAGNOSIS
Ultrasound
- The hCG level at which an intrauterine pregnancy should be seen on transvaginal US is referred to as the discriminatory zone.
- An intrauterine gestational sac will be detected at a hCG level of 3510 mIU per mL with 99% probability (Connolly 2013).
- A gestational sac is rarely visualized in an early pregnancy <35 days from LMP, and therefore not expected. Follow up US in 7 days with ectopic precautions is appropriate management for PUL < 35 days, if not managed with diagnostic aspiration.
- Serial serum hCG levels can be utilized in addition to US for PUL evaluation, especially if hCG level is below discriminatory zone.
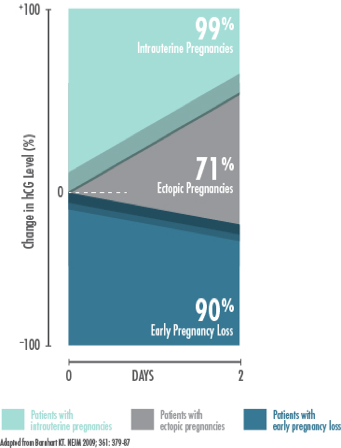
- A viable IUP typically has an hCG trend characterized by an expected hCG increase of 53% over 48 hours, however this trend can be as slow as a 35% increase in 48 hours (Butts 2013, Prine 2011). While using a threshold of a 53% increase is 99% sensitive for detecting viable IUPs, consider using a lower threshold in patients with desired pregnancies to avoid misclassification of an early IUP as an ectopic or EPL.
- The rate of hCG increase and trends may be unpredictable, especially at low levels. Three serial hCGs are typically needed to establish a trend, typically on days 0, 2, and day 4 or 7. The change in hCG level for patients experiencing an IUP, ectopic pregnancy, or EPL is quite nuanced, and hCG levels must always be correlated with the full clinical picture.
- The minimum rate of decline expected for EPL depends on the initial hCG at presentation, but it ranges from 35-50% at 2 days (Butts 2013).
- Rate of hCG rise with ectopic is usually slower than expected for a viable IUP.
- Among patients diagnosed with ectopic pregnancies:
- The majority had serial hCG rise below the normal range for a viable IUP (i.e. level rose < 35-53% in 2 days).
- For those with declining hCG, the rate of decline is usually slower than that expected for EPL.
- However, 21% of ectopics have a hCG rise similar to viable IUP and 8% have a decrease that is normal for EPL (Silva 2006).
- Therefore, use caution when following patients in early pregnancy with possible symptoms of ectopic pregnancy, i.e. intermittent bleeding/spotting, pelvic pain.
- A “normal” rise or fall in levels is not sufficient to exclude ectopic – but should be used in conjunction with other clinical data including exam, US or diagnostic aspiration.
PUL MANAGEMENT
A patient-centered approach, prioritizing desired pregnancy outcome, can be used to guide decision-making and approach to managing a pregnancy of unknown location (Flynn 2020).
- If patient desires to terminate the pregnancy, management options include:
- Medication Abortion: various protocols allow MAB in setting of PUL with ectopic precautions & serum hCG trend to confirm completion (Goldberg 2022).
- Diagnostic Uterine Aspiration: can be offered at same visit of PUL identification, if pregnancy tissue (gestational sac or villi) found in aspirate, an ectopic pregnancy is ruled out and management is complete. If no pregnancy tissue identified, review ectopic precautions, collect hCG, and trend with repeat hCG in 24-48 hours until able to confirm diagnosis of completed abortion or ectopic pregnancy. Referral for ectopic pregnancy management is warranted if patient becomes symptomatic or if hCG does not drop by 50%.
- Methotrexate: Methotrexate 50 mg/m2 can be effective in treating early ectopic pregnancy when the diagnosis of viable IUP or EPL cannot be confirmed (persistent PUL) if criteria are met. Managing a persistent PUL with methotrexate or uterine aspiration is more likely to result in a successful pregnancy resolution compared to expectant management (Barnhart 2021). Efficacy is determined with serial hCG testing, clinical exams and progression of signs and symptoms. (Seeber 2006)
- If patient desires to continue the pregnancy:
- Serial hCG and / or US to continue evaluation for diagnosis of EPL or ectopic. If EPL or ectopic is conclusively diagnosed, offer appropriate management and / or referral (see Chapter 8 Management of EPL, RHAP Diagnosis and Treatment of Ectopic Pregnancy).